EHR Software Development

Your Budget, Simplified - Discover Your Project's Cost
Choose your industry
What’s your business goal?
Specify the date to release your project
Choose your platform
How big is your app?
Do you need custom designs for your app?
Cloud infrastructure provider
What features should your app have?
Additional information
When do you want to start?

Future-Proof Your Practice with Custom EHR Development
EMR/EHR Solutions for Faster Intakes & Smarter Follow-Ups
Serve More Patients with the Same Team
- Reduce chart filing time by up to 54%
- Improve appointment scheduling by up to 28%
- Lower staff time on results by up to 32%
Functionalities for Better Care
- PHI & history storage
- Vaccine tracking
- Appointment reminders
- Patient access point
- Smart templates & e-forms
- All-in-one dashboards
- Task tracking & reminders
- Practice management tools
- Symptom pattern visuals
- Condition changes scenarios
- Treatment reports
- Referral & activity analysis
- Multi-factor authentication
- Role-based access control
- Encrypted data storage
- Secure transfer protocols
- Voice recognition tools
- AI chatbots & assistants
- E-prescription support
- Medical device integration
- Medical billing integration
- Financial dashboards
- Automated payment reminders
- Insurance eligibility checks
Care-Driven EHR Development Services
EHR Solutions for All Care Settings
EHR or EMR? Make the Right Choice for Your Practice
Bring It All Together with EHR Integration
Your Path to a Custom EHR/EMR Solution
What our clients say about us
Success Stories
Who we are
About usGlorium Technologies is a full-cycle app & software development company which covers specific client business needs and manage them with the help of the best possible technology solutions.
Since 2010, we have been inventing digital breakthroughs, helping startups and businesses come out on top in their markets.

Why choose us
Let's Connect!
A Complete Guide to Custom EHR Software Development for Modern Healthcare
Healthcare organizations have long started optimizing their technology adoption to improve patient experience, comply with regulations, and stay ahead of the competition. Munich Re Life U.S. survey, conducted in 2022, highlights the growth of EHR software, reporting a rise of 38%. We saw even more growth in the following years, and experts predict that even more healthcare facilities will adopt EHR and EMR software.
Why does this happen? Well, for starters, healthcare companies want to improve their patient data collection, assessment, and usage methods, optimize their workflows, and comply with regulatory standards. On the other hand, an increased number of ransomware attacks on healthcare organizations (67% in the U.S. in 2024, according to Statista) urges companies to opt for encrypted cloud computing and security measures.
Long story short, EHR software development opens doors to many opportunities. Of course, there are challenges and specific processes for EHR adoption, and that’s what we want to explore in this article.
A Look at the Current Market Landscape of EHR Development
Electronic health records are a must-have and in great demand in modern medical practice. In its market research report, Grand View Research valued the EHR market at $33 billion. Even with the growth and development of new healthcare solutions, the basic purposes of applications have not changed. However, the existing software systems still do not fully satisfy the users’ unique needs and requirements.
About 42% of doctors and healthcare professionals have stated that they are unsatisfied with the current EHR software. The pandemic and the growing digitalization require improved, interconnected, secure, and effective EHR and billing software.
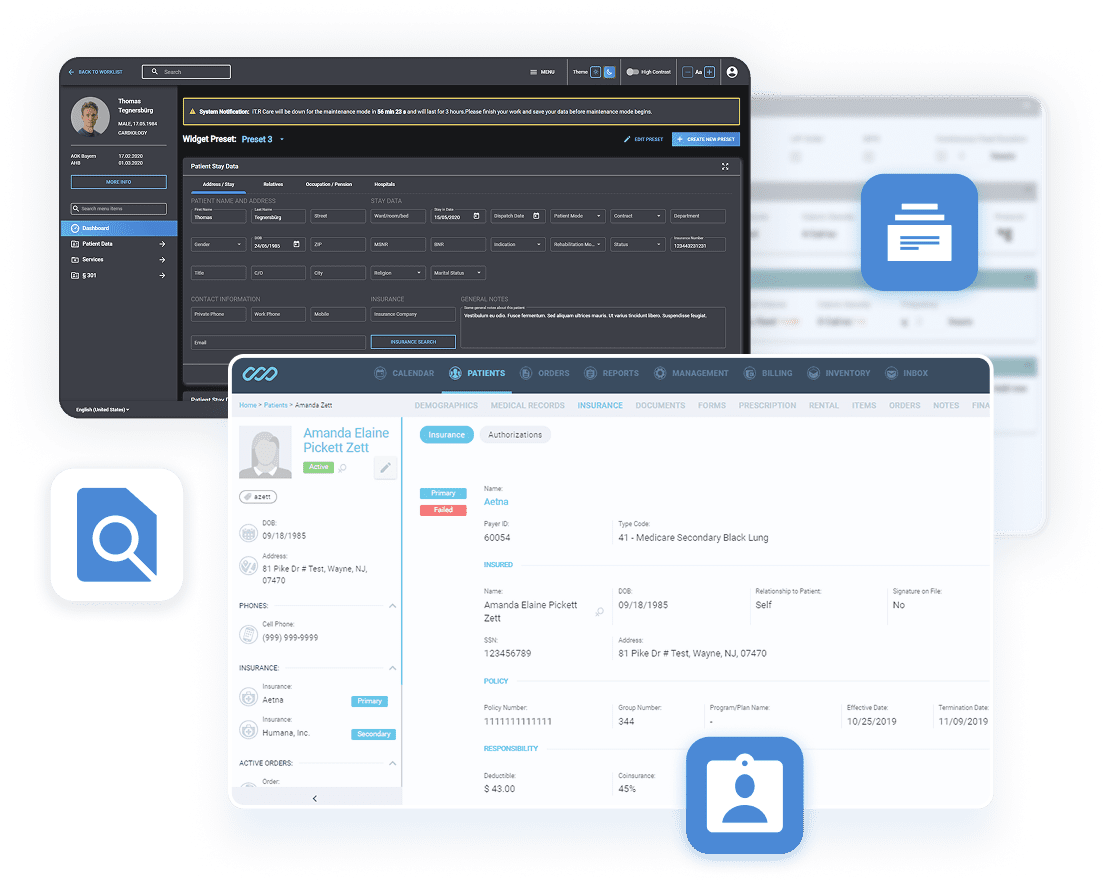
So, what is an EHR system? We don’t usually include theoretical explanations and boring content, but electronic health record systems are complex necessities, so we need to explore them a bit more.
EHRs are centralized, real-time patient health records created for easy data access and retrieval. They gather and organize patient medical information, which helps healthcare companies oversee and analyze this clinical data for a better patient experience.
EHRs can store the data on:
- Medical history
- Diagnoses
- Medications
- Immunization dates
- Allergies
- Radiology images
- Test results
- Demographic and billing data
An EHR system can also communicate with other healthcare entities. It can encompass all forms of facilities like ERs, labs, specialists, diagnostic centers, pharmacies, and workplace clinics, and thus, they are part of the patient journey.
Types of EHR/EMR integration solutions
Since you’re looking for suitable EHR software for your company, we recommend first exploring the categories of EHRs based on their features, deployment methods, and service scopes:
- On-premise EHRs: On-premise EHRs are hosted on the provider’s server and are maintained by the provider’s IT department. Such EHRs will provide you with an opportunity to customize them; you will own the data and integrate it with other systems easily. Keep in mind that they also require significant capital investment in software, hardware, and personnel
- Cloud-based EHRs: Cloud-based or SaaS EHRs, which are stored on the vendor’s server and accessed through the internet, are relatively cheaper to implement with a subscription-based model. They are scalable and can be accessed remotely, but are not very customizable and depend on a stable internet connection
- Integrated EHRs: EHRs are designed to contain practice management functions such as billing, scheduling systems, or patient portals to help manage administrative duties and ensure seamless data exchange. Different providers offer different EHR integration levels, so the cost will vary
Understanding these categories will help you better assess which EHR type aligns with your operational needs, technical capacity, and long-term goals.
Benefits of EHR system development and implementation
Selecting the correct category and adhering to the steps in the EHR development process will allow your organization to optimize its processes, increase market position, and increase the overall effectiveness of business processes.
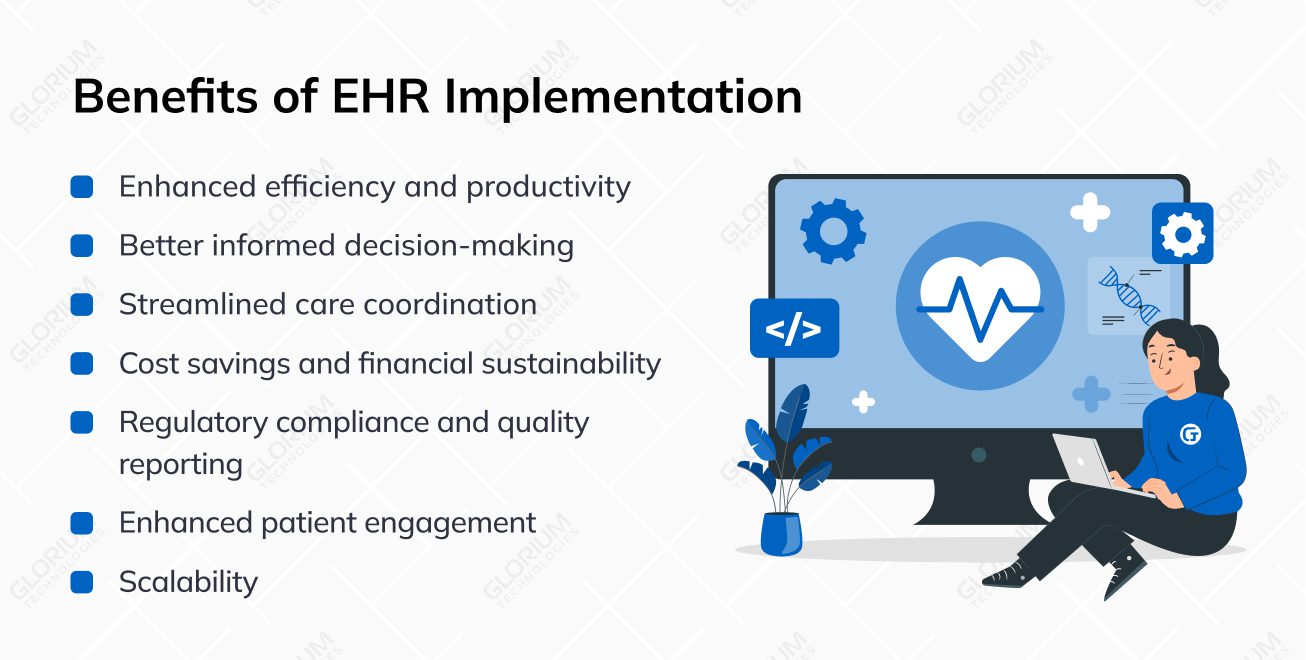
- Enhanced efficiency and productivity: EHRs allow for the automation of tasks such as appointments, orders, prescriptions, and billing, which means that the workforce can attend to patients. EHR developers can also help you increase efficiency and allow more focus on the patient instead of paperwork or non-nursing tasks
- Better informed decision-making: EHR software provides healthcare organizations with details of patients’ medical history, such as allergies, treatment plans, diagnoses, and lab results. Hence, this data enables informed decision-making, which is vital for patient outcomes
- Streamlined care coordination: Robust EHR software makes it easier to transfer patient data across the different providers, departments, and institutions, thus improving care coordination
- Cost savings and financial sustainability: Although there is an initial outlay to acquire EHR software, it is cost-effective in the long run due to reduced costs on paperwork, such as printing and filing
- Regulatory compliance and quality reporting: Healthcare enterprises are subject to significant regulatory requirements and increasing standards concerning quality measures. EHR/EMR integration helps providers meet these measures and improve the quality of reporting
- Enhanced patient engagement: EHR has a patient portal where patients can access their medical records, book an appointment, request a prescription refill, and communicate with the provider, educating patients and increasing the level of their engagement
Therefore, EHR software implementation supports clinical excellence and operational efficiency, positioning your organization for sustainable growth and innovation in healthcare delivery.
Features That Justify the EHR Software Development Cost
Numerous EHR software features help in improving the efficiency of the clinical processes and meeting the legal requirements. Here are the key EHR capabilities to consider when evaluating or developing a medical system:
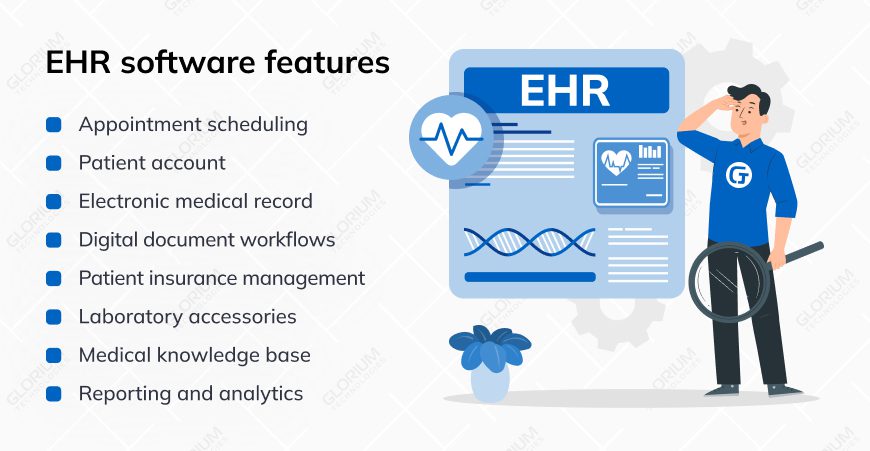
- Appointment scheduling: This feature promotes real-time viewing and editing of provider schedules, appointment bookings, and even reminders. This eliminates most of the paperwork in healthcare facilities and, in turn, improves patient satisfaction
- Patient account: Adding this feature will dramatically improve the patient onboarding process
- Electronic medical records: Enables medical documentation of examinations such as initial examination, epicrisis, and diary entries, registration of patient diagnostic data, and registration and storage of medical appointments
- Digital document workflows: Everything from the patient intake and medical consent forms to different agreements has to be done digitally
- Patient insurance management: Enhances business process management with insurance companies
- Laboratory accessories: Help in the automation of communication within a laboratory, as all information is synchronized with a patient’s profile
- Medical knowledge base: Allows doctors to have the updated treatment and diagnostic guidelines they need
Custom EHR Software Development: Challenges and Solutions
Even though EHR/EMR systems are aimed at optimizing the work of healthcare organizations, introducing such a system is not without considerable pitfalls.
Healthcare regulation compliance
Challenge: In healthcare, the legal frameworks that influence EHRs include GDPR and HIPAA regulations, which address issues related to patient privacy, data security, integration, and communication. HIPAA compliance is a must, as any violation attracts severe penalties.
Solution: Partner up with custom EHR software development companies that are conversant with the regulations. They create systems that address legal frameworks and change software as required. Properly educating employees on regulatory requirements helps minimize risk and ensures better compliance.
Interoperability issues
Challenge: Although health information exchange standards exist, EHRs experience data sharing difficulties, resulting in incomplete patient information.
Solution: It can be helpful to select an EHR system that is compatible with interoperability standards, such as HL7 or FHIR. Moreover, cooperation with other healthcare providers and IT suppliers can improve data exchange.
Usability and training
Challenge: It is not uncommon to hear that EHR systems are hard to use and this makes the healthcare providers unproductive and unhappy. This can be due to the fact that the interface is too complicated.
Solution: Choosing custom software with a smooth and easy-to-use interface can help avoid this problem. Also, routine and extensive training should be offered to all users of the EHR system to enable them to use it properly.
Data security and privacy
Challenge: EHR systems contain patients’ information and are vulnerable to cyber threats. Data breaches can have dire legal and financial implications and can damage the organization’s credibility.
Solution: Some important measures include encryption, secure user authentication, and regular security audits. In addition, security practices for the staff and keeping all the software updated can also help minimize the risk.
High implementation costs
Challenge: Acquiring and implementing an EHR system is costly, as it involves software, hardware, staff training, and general upkeep.
Solution: Cloud-based EHR systems may be less expensive in terms of initial investment and more suitable for small practices. Strategic and financial management can also be used to achieve the desired return on investment.
With a correctly implemented EHR system, your company will feature a competitive advantage:

Many hospitals have adopted EHR/EMR software solutions. However, there are implementation issues – patients and staff struggle with new applications and programs.
To address this problem, healthcare software developers pay close attention to the design of certain features, which are intended to facilitate integration and increase the product’s appeal.
What a Medical Billing Solution Needs for Effective EHR/EMR Data Integration
The billing process is a crucial aspect of healthcare services; therefore, it becomes essential to have a proper system that can handle claims, code management, and analytics in medical practice.
Advanced billing systems manage the creation of billing documents and charge posting, which means that financial processes are accelerated and monotonous tasks are eliminated.
Integration with billing and financial management software
The first important aspect of medical billing software should be an adaptable and interactive integration that allows for efficient financial work in an EHR system to be done.
If there is no proper way to link the system with an EHR system, the billing process will be very cumbersome—this is not the intended goal.
Tracking & processing of the medical billing codes
HCPCS and CPT are vital code sets in medical billing. Every service that a clinician offers is assigned a code to help with tracking and billing. These codes also set the rate of reimbursement by health insurance organizations.
Thus, coding errors cost healthcare organizations approximately $15.95 billion, according to the CMS. Disclosing the 2019 figure, the organization said it dealt with $1.73 billion in incorrect payments. Thus, it is crucial for medical software to provide compliant, accurate code lists and make code assignment and processing a part of the system’s operations.
Medical claims management
One of the most important functions of custom healthcare solutions is to manage and control medical claims. Medical billing software is a system that handles the submission of claims and even notifies the parties that have been rendered the services in cases where claims are denied; it handles claim reconciliation and many other things.
Appointment scheduling system
All reliable medical billing software should be equipped with powerful scheduling features to help organize the communication process between patients and clinicians, ensuring effective remote patient monitoring. An easy-to-access interface will enable clinicians and patients to schedule appointments, check their appointment histories, and view the doctor’s notes. This critical feature should also encompass recognizing the wrongly assigned code and, if possible, providing an automatic response.
Financial reporting
Having access to the patient data, which is linked to the billing history, allows for preparing a solid financial report. Effective EHR systems enable the analysis of patient data and real-time financial reports, which can lead to valuable suggestions for enhancing patient comfort.
Interoperability Standards: The Backbone of Modern EHR Development
Building a custom EHR system that works in isolation defeats the purpose. Your platform needs to exchange data reliably with labs, pharmacies, insurance payers, public health agencies, and other provider organizations. That’s where interoperability standards come in, and getting them right from the start separates a functional EHR from one that creates new data silos.
HL7 FHIR: The current gold standard
Fast Healthcare Interoperability Resources (FHIR), developed by Health Level Seven International, has become the dominant standard for healthcare data exchange. Unlike its predecessor, HL7 v2 (which still powers many legacy interfaces), FHIR uses RESTful APIs and modern web formats such as JSON and XML. This makes it significantly easier for developers to build, test, and maintain integrations.
Why does this matter for your project? The ONC’s 21st Century Cures Act Final Rule requires certified EHR systems to support FHIR-based APIs, specifically the USCDI (United States Core Data for Interoperability) dataset. If your custom EHR will pursue ONC certification, or if you need to connect with any certified system that has it, FHIR capability is not optional. It’s a regulatory baseline.
In practice, FHIR resources cover everything from Patient and Observation to MedicationRequest and DiagnosticReport. Your development team should map your clinical workflows to these resource types early in the discovery phase. Retrofitting FHIR compliance after launch is far more expensive than architecting it from the ground up, which is why any experienced EMR software development company will prioritize FHIR architecture from day one.
Other standards you’ll encounter
FHIR handles a lot, but real-world EHR interoperability involves a stack of complementary standards:
- HL7 v2 messaging still dominates lab interfaces, ADT (Admit, Discharge, Transfer) feeds, and pharmacy communications. Many hospitals and reference labs have not migrated to FHIR, so your EHR will likely need a v2 engine for backward compatibility
- C-CDA (Consolidated Clinical Document Architecture) is the standard format for care summaries exchanged during transitions of care. Think discharge summaries, referral notes, and continuity of care documents
- IHE profiles (Integrating the Healthcare Enterprise) define specific implementation guides for scenarios like cross-community document sharing (XCA) and patient identifier matching (PIX/PDQ). If your EHR serves multi-site networks or participates in health information exchanges (HIEs), IHE conformance is critical
- DICOM (Digital Imaging and Communications in Medicine). If your EHR integrates with radiology or pathology systems, supporting DICOM queries and image references prevents your clinicians from toggling between disconnected viewers
What information blocking rule mean for your build
The ONC’s information blocking regulations prohibit practices that interfere with the access, exchange, or use of electronic health information. This applies to healthcare providers, certified health IT developers, and health information exchanges alike.
For your custom EHR, this means you must provide patients and authorized third parties with standardized API access to their health data. You cannot impose unnecessary technical barriers, charge unreasonable fees for data access, or restrict exports to proprietary formats. Violations carry real penalties, so your EHR software development company should build compliance into the architecture, not treat it as a checkbox during QA.
Practical steps to get interoperability right
Start with an integration audit during discovery. Catalog every external system your organization currently exchanges data with, including the format, frequency, and direction of each data flow. Then prioritize: which connections are day-one requirements, and which can roll out in later phases?
Your development team should also implement a robust API gateway to manage authentication, rate limiting, and logging for all external connections. Standardizing on OAuth 2.0 and SMART on FHIR for authorization ensures secure, granular access control that aligns with both HIPAA and ONC requirements.
Finally, plan for testing with real trading partners early. Synthetic data only goes so far. Coordinating connectivity testing with your labs, imaging centers, and HIE network before go-live prevents the integration failures that derail so many EHR launches. A thorough approach to EMR software development accounts for these real-world testing scenarios well before deployment day.
Your Practical Roadmap to Building EHR Software
Building a healthcare system is a significant initiative involving a combination of strategic planning, technical expertise, user involvement, and regulatory compliance. Here’s a step-by-step guide to developing a robust and effective EHR software system:
Define your goals and objectives
Your goals may include increasing the efficiency of clinical activities, patient care, invoicing, or fulfilling legal requirements. Be specific, and make sure they are linked to the general organizational strategy.
Assemble a cross-functional team
Implementing EHR software is not a one-man job, so the involvement of multiple stakeholders is crucial. These stakeholders should include clinical personnel who will work with the system, IT personnel who can provide technical support, managers who can address the organizational requirements, and legal specialists who can explain matters of the law.
Understand user needs and workflows
Take time to learn your target users’ application usage patterns. What are the current practices regarding patient data management? What difficulties do they have? What would the users most likely consider to be the most useful? This paper shows that end-user participation is vital in designing an EHR solution that will be valuable to the users.
Select the right technology stack
Your tech stack will hinge on several factors, including the resources you have at your disposal, including financial, temporal, and specific features that you want to incorporate. It is also important to consider how the system is to be deployed, either through the cloud or on the organization’s physical infrastructure, with all the benefits and drawbacks that come with each.
When selecting a technology stack, it’s important to choose technologies that have a strong track record and remain relevant in the future. This can save you from needing to redevelop your system down the line due to outdated technology.
Electronic health record systems often need to integrate with other systems such as lab information systems, radiology information systems, and billing systems. Your technology stack should support these integrations.
A few examples of technologies commonly used in EHR software development include:
- Backend Languages: Python, Java, C#, Node.js
- Frontend Frameworks: AngularJS, React, Vue.js
- Databases: MySQL, PostgreSQL, MongoDB
- Mobile Development: React Native, Swift (for iOS), Kotlin (for Android)
Anton KumechkoProject Manager, Glorium Technologies
Design a user-friendly interface
EHR systems are commonly implemented inadequately because they are hard to use. Collaborate with people who have a professional background in UI/UX design, focusing on healthcare applications.
Implement key EHR features
Ensure that the key functionalities of the system include patient handling, clinical documentation, prescription management, laboratory integration, health information exchange, billing and coding, patient portal, reporting and analysis, appointment scheduling, and interoperability.
Ensure regulatory compliance
Collaborate with professionals who have training and certification in healthcare regulations and standards.
Develop robust security measures
Ensure that patient data within EHRs is protected by secure user authentication, data encryption, security checks, and data backup and recovery procedures, among other measures.
Conduct thorough testing
Before launching your EMR system, conduct thorough testing to identify and resolve issues while ensuring proper functionality, performance, usability, and security.
Maintenance and training
It is always a discomfort when a new EHR system is suddenly introduced into the practice. Phasing the implementation is advisable, beginning with a selected group and then with the entire employee population.
How to Choose a Reliable EHR Software Development Company?
Selecting the right EHR development company is a strategic decision that can affect the quality of your healthcare services. A good EMR/EHR software development partner can enable you to provide quality patient care through proper data management and smooth operation. The market is saturated with vendors, but we can give you a little guide on how to choose a reliable EHR development company:
Industry expertise: Choose a company with extensive experience in EHR software development. They should know how the healthcare industry functions and the related rules so that they can meet your EHR implementation needs. Assess their performance history, healthcare project experience, and knowledge of today’s healthcare technologies.
Reviews and client testimonials: By reading the testimonials of previous clients, you’ll be able to gain some understanding of the company’s previous work in EHR software development, adherence to timelines, and costs, among other factors. Look at their website, LinkedIn page, and other resources. You can find our client’s success stories and testimonials here.
Cost-effectiveness: Though the cost of EHR software development should not be the only consideration when it comes to making a selection of EMR software developers, it is an important factor that cannot be ignored.
Don’t go for the lowest price in the market, as this may lead to low-quality custom EHR solutions, error-prone data migration, and long-term costs from constant rework. Choose a company that offers clear pricing based on the quality of EMR software development services they offer. Determine what is encompassed in the fee, such as development, post-deployment support, maintenance, training, customization, or data transfer.
Communication aspects: Effective and transparent communication is essential throughout the custom EHR development lifecycle. Choose a company that provides regular updates, clear documentation, and direct access to project managers or lead developers. They should be proactive in addressing your questions, aligning with your internal stakeholders, and adapting to evolving requirements.
By partnering with Glorium Technologies for your EHR software development needs, you can leverage our technical expertise, healthcare IT knowledge, and commitment to quality. Contact us and create an EHR system that truly adds value to your healthcare organization.
Questions You May Have
How does Glorium Technologies protect your idea as an EMR software development company?
We are strongly committed to protecting your privacy. As stated on all our services pages and during our first communication, we use NDAs (non-disclosure agreements) to protect your data and intellectual property during the whole EHR software development project.
Why is EHR/EMR software development important for healthcare providers?
EHR software development is crucial for healthcare providers as it facilitates improved patient care, enhances productivity, and helps reduce the potential for errors. It streamlines medical data management, enables easy access to patient records, and aids in decision making. Additionally, it promotes coordinated care by allowing information sharing across different healthcare providers.
What are the key considerations for effective EMR system integration?
To achieve effective EMR system integration, you should focus on data accuracy, interoperability, and regulatory compliance. User-friendly design, secure data exchange, and minimal workflow disruption are also important. Engaging clinical staff early helps ensure adoption and supports long-term success across the organization.
Can your EHR support EMR data integration with other systems?
We vouch for seamless integration so that you can benefit from efficient workflows, accurate data sharing, and better patient care. We ensure your EHR system can connect with lab software, imaging tools, and other third-party platforms to avoid data silos and streamline clinical and administrative processes.
What should healthcare providers look for when choosing EMR integration services?
You should seek proven interoperability, compliance with HL7 and HIPAA, secure data handling, and compatibility with existing systems. Responsive support, customization options, and experience with various medical software platforms are essential for smooth implementation and long-term efficiency.